The Challenge of the 15-Minute Consultation
If you suffer from chronic migraines, you know how crucial a good neurologist is. You wait months for an appointment, driving for hours to reach a specialist clinic. Yet, when you finally get into the exam room, you often have just 10 to 15 minutes to convey months of debilitating pain.
If you show up with vague memories—"I think I had about ten headaches last month, and they were really bad"—your doctor lacks the clinical foundation required to prescribe modern preventative treatments or justify expensive interventions like CGRP inhibitors to your insurance company.
To maximize your consultation and get the most effective treatment plan, you must learn how to present migraine data to a neurologist properly.
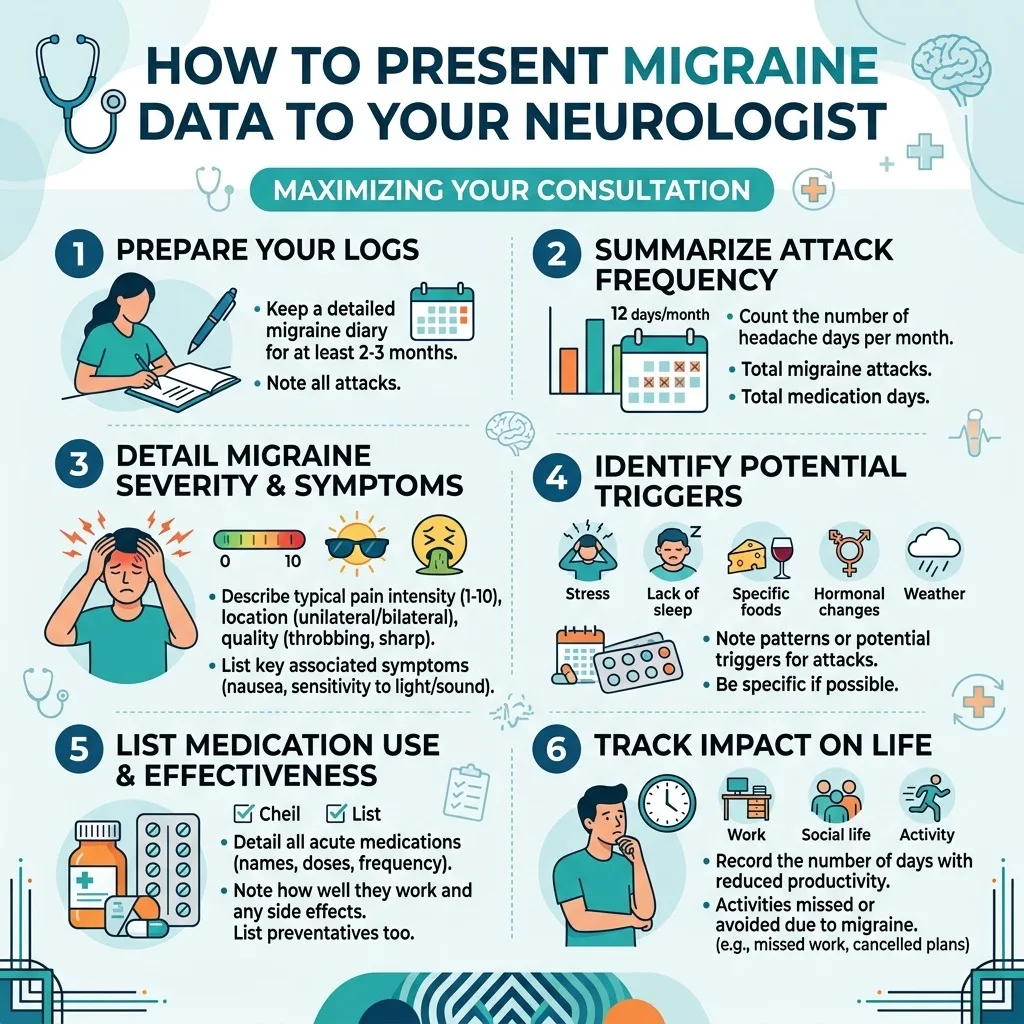
What Neurologists Actually Need to Know
Neurologists rely entirely on patient-reported data to diagnose primary headache disorders. Unlike broken bones or infections, there is no blood test or MRI scan that definitively "proves" a migraine. Your data is the diagnostic tool.
When reviewing your history, a headache specialist looks for specific metrics. Here is exactly what they need:
1. Attack Frequency and Duration
The single most important metric is your Monthly Headache Days (MHD) versus Monthly Migraine Days (MMD).
- Frequency: "I had 14 headache days last month; 8 of those met migraine criteria."
- Duration: "Untreated, my attacks last 24 to 48 hours."
- Why it matters: This data is the primary factor in determining if you suffer from episodic or chronic migraine (defined as 15+ headache days per month, with at least 8 being migraines). It dictates which preventative medications insurance will cover.
2. Pain Characteristics and Symptoms
A precise description of the pain helps differentiate migraines from cluster headaches or tension headaches.
- Location: Unilateral (one side), bilateral, frontal, base of skull.
- Quality: Throbbing, pulsating, stabbing, dull ache.
- Severity: Utilizing a standard 1-10 pain scale.
- Associated Symptoms: Nausea, vomiting, photophobia (light sensitivity), phonophobia (sound sensitivity), allodynia (pain from normal touch).
- Presence of Aura: Visual disturbances, tingling, or speech issues prior to the headache phase.
3. Medication Use and Efficacy
Your doctor needs a precise accounting of what you are taking, how much, and if it is actually working.
- Acute Medications: Triptans, NSAIDs, gepants. Did you achieve pain freedom at 2 hours?
- Frequency of Use: "I took sumatriptan on 12 different days last month."
- Why it matters: Utilizing acute medications more than 9-10 days a month puts you at severe risk for Medication Overuse Headache (MOH), also known as rebound headaches. Your doctor must monitor this closely.
4. Functional Impairment
How much does the migraine prevent you from living your life?
- Impact: Days of work missed, social events cancelled, or days spent bedridden in a dark room.
- Why it matters: Doctors use standardized questionnaires like the MIDAS (Migraine Disability Assessment) or HIT-6 to measure disease burden and justify aggressive treatment pathways.
How to Structure and Present Your Data
Arriving with months of raw, handwritten journal entries is almost as bad as arriving with no data at all. A physician cannot synthesize six months of scribbled daily notes in an 8-minute window. Your data must be structured, aggregated, and synthesized.
Step 1: Use a Digital Tracking App
Stop relying on memory or paper logs. Use a dedicated tool like the Migraine Trail app to record attacks as they happen. An app ensures data standardization and eliminates the risk of forgetting crucial details.
Step 2: Generate an Aggregated Clinical Report
Instead of showing your doctor a calendar, generate an aggregated summary. At the click of a button, Migraine Trail produces a comprehensive Neurologist Report. This PDF instantly visualizes:
- A rolling 90-day chart of attack frequency.
- A percentage breakdown of symptom occurrence (e.g., Nausea presents in 85% of attacks).
- A clear timeline of medication usage versus attack severity.
Step 3: Lead with the Summary
When the doctor asks, "How have you been?", do not start with a chronological story. Start with the data-driven summary:
"Since our last visit 3 months ago, my frequency has increased. I am averaging 12 migraine days a month, up from 8. My acute medication, sumatriptan, is only providing pain relief about 40% of the time, and I am starting to miss sleep due to severe nighttime attacks. Here is my 90-day tracking report."
By leading with hard statistics, you immediately establish the severity of your condition and frame the rest of the conversation around finding solutions.
The Importance of High-Fidelity Data Entry
To generate great reports, you must input accurate data. However, logging data during an attack is incredibly difficult. Looking at a bright screen to tap out symptoms when experiencing severe photophobia is agonizing.
This is where integrating technology like voice logging becomes essential. Using the Migraine Trail app, you can lay in a completely dark room and simply speak into your phone to log your attack. The AI instantly categorizes your symptoms, severity, and timestamps. This ensures you capture the most accurate data at the peak of the attack, resulting in much higher fidelity reports for your provider.
Summary
Presenting your migraine data effectively transforms you from a passive patient into an active partner in your healthcare. By diligently tracking your symptoms and utilizing technology to aggregate that data into clinical reports, you empower your neurologist to make rapid, accurate, and life-changing treatment decisions. Download a modern tracking app today and start taking control of your clinical narrative.